When you stop or cut back on a substance your body has gotten used to, it has to adjust. The physical and psychological effects you feel during this adjustment period are what we call withdrawal symptoms. Think of it as your body's way of re-learning how to work without something it has come to depend on.
Key Takeaways
- Withdrawal is a biological process: It's the body's natural, predictable reaction to the absence of a substance it has become dependent on, not a sign of weakness.
- Symptoms vary by substance: Different drugs affect the brain in unique ways, leading to distinct withdrawal experiences. Symptoms for alcohol are different from opioids or stimulants.
- Safety is paramount: Withdrawing from certain substances like alcohol and benzodiazepines can be life-threatening. Medical supervision is essential in these cases to manage severe symptoms like seizures.
- Recovery is a two-stage process: After the initial, intense acute phase, many people experience Post-Acute Withdrawal Syndrome (PAWS), which involves longer-lasting psychological and emotional symptoms.
Unpacking the Body's Recalibration Process
Imagine your body is constantly working to maintain a perfect internal balance, a state scientists call homeostasis. It’s like having a very precise internal thermostat. When you consistently use a substance, whether it's alcohol, opioids, or even caffeine, you're essentially overriding that thermostat.
Your body, ever adaptable, eventually stops fighting it. It just accepts the substance as part of the new normal and adjusts its entire system to function with it.
So, what happens when you take that substance away? The whole system gets thrown into chaos. The thermostat that was relying on an external chemical to stay steady is now swinging wildly, trying to find its original set point. This intense, sometimes jarring, recalibration process is what triggers withdrawal symptoms. It’s the body’s alarm system screaming that something is wrong.
To really get a handle on this, it's helpful to break down the key ideas.
Core Concepts of Withdrawal Explained
| Concept | Simple Explanation | Real-World Example |
|---|---|---|
| Dependence | Your body has adapted to a substance and needs it to feel "normal" and avoid withdrawal symptoms. | A heavy coffee drinker who gets a splitting headache and feels sluggish if they miss their morning cup. |
| Homeostasis | Your body's natural state of internal balance. It controls things like temperature, heart rate, and brain chemistry. | When you get hot, you sweat to cool down. When you're cold, you shiver to warm up. That's homeostasis in action. |
| Recalibration | The period where your body tries to return to its natural balance (homeostasis) after a substance is removed. | After quitting nicotine, the brain has to re-learn how to produce its own "feel-good" chemicals without the constant stimulation from cigarettes. |
Understanding these terms helps frame withdrawal not as a moral failing, but as a predictable biological process.
Physical vs. Psychological Dependence
Withdrawal isn't just one thing; it usually hits on two fronts at once.
-
Physical Dependence: This is all about the body. Your cells have literally changed to accommodate the substance. When it's gone, you feel it physically—think shaking hands, nausea, sweating, or a racing heart.
-
Psychological Dependence: This is the mental and emotional side of the coin. It's the intense cravings, the sudden mood swings, the crushing anxiety, or the irritability that pops up when you can't use the substance. It’s your brain missing the chemical it learned to associate with pleasure or relief.
These two types of dependence are almost always intertwined, creating a unique and complex experience for each person. The chances of experiencing withdrawal also vary wildly depending on the substance.
For example, about 18.4% of adults who drink heavily and 15.2% of daily smokers report withdrawal symptoms. For other substances, the numbers are much lower—around 0.37% for opioids and 0.35% for cocaine, according to data available from the National Center for Biotechnology Information.
In essence, withdrawal is not a sign of weakness but a biological response. It is the challenging but necessary journey your body takes to restore its natural equilibrium after a period of chemical dependence.
Ultimately, everyone's experience is different. The substance you used, how long you used it, and your overall health all play a huge role in what your withdrawal will look and feel like. Knowing this helps you see the process for what it is: a tough but manageable step toward recovery.
The Science of Why Your Body Reacts

To really get a handle on what withdrawal symptoms are, you first have to appreciate the incredible balancing act your body pulls off every single second. This state of internal stability has a name: homeostasis. Keeping everything in balance is your brain's most important job.
Imagine your brain is a master sound engineer at a mixing board, constantly tweaking countless faders to keep everything sounding perfect. It manages your mood, energy levels, and even your perception of pain by carefully releasing chemicals called neurotransmitters.
Now, what happens when a substance like alcohol or an opioid enters the picture? It’s like someone hijacking the soundboard and cranking the volume on the "feel-good" tracks way past their natural limits. At first, your brain tries to compensate by turning its own internal volume down. But if this happens over and over, it eventually adapts. It starts producing fewer of its own feel-good chemicals and lets the substance do all the heavy lifting. A new, fragile balance is struck.
Your Brain on Overdrive
The real trouble begins when that substance is suddenly taken away. The sound engineer—your brain—is left with all its internal dials turned way down, but the powerful external chemical that was boosting the signal is gone. The result is pure static. The system is thrown completely out of whack.
In a frantic attempt to get things back to normal, the brain overcorrects in a big way. It floods your body with adrenaline and other stress chemicals, which is precisely why the early stages of withdrawal often feel like a severe anxiety attack or a state of sheer panic.
This sudden rebound effect is the very heart of withdrawal. It's not a moral failing or a sign of weakness; it's a predictable neurochemical storm that erupts when a brain that has adapted to a substance is forced to function without it.
This biological scramble is what triggers the intense physical and psychological reactions we call withdrawal symptoms. Your body is just trying to find its footing again without the chemical crutch it came to rely on.
The Rubber Band Analogy
Here’s a simple way to picture what’s happening. Think of a rubber band. Consistent substance use is like stretching that rubber band farther and farther away from its natural, relaxed state. Over time, your brain gets used to this new tension and starts treating it as the new normal.
Stopping "cold turkey" is like suddenly letting go of that stretched rubber band. It doesn’t just gently drift back to its original shape—it snaps back violently. That "snap" is the withdrawal experience. It’s a chaotic over-correction that produces symptoms like shaking, sweating, anxiety, and powerful cravings. The further the band was stretched (i.e., the longer and heavier the substance use), the more powerful that snap back will be.
Physical vs. Psychological Dependence
This intense reaction really shines a light on two different, yet deeply connected, types of dependence. Understanding both is key to seeing the full picture of withdrawal.
-
Physical Dependence: This is the "rubber band snap" in action. Your body's actual cells and brain chemistry have changed to accommodate the substance. When it’s removed, the body protests with very real, tangible symptoms: nausea, tremors, muscle aches, and crushing fatigue. It’s not just that your body misses the substance; it physically needs it to function without feeling sick.
-
Psychological Dependence: This side of the coin lives in your thoughts, emotions, and behaviors. It’s the nagging, overwhelming craving and the compulsion to use again, not just to feel good, but to escape feeling bad. This is driven by the brain's reward pathways, which have been rewired to scream that the substance is essential for survival and well-being.
When you put these two forces together, you get a perfect storm. The physical symptoms make you feel terrible, while the psychological dependence whispers that there’s a quick, easy fix to make it all stop. This is what makes getting through withdrawal so incredibly difficult and why professional support can be a true lifeline.
Common Symptoms by Substance Type
While the core experience of withdrawal is something many people share, the exact symptoms you'll face depend heavily on the specific substance involved. Think of it this way: different substances have their own unique "fingerprint" on your brain's chemistry. When you stop using them, the brain's attempt to get back to normal produces a distinct set of physical and psychological effects.
Knowing what to expect is more than just academic—it's a critical part of staying safe. The process of withdrawing from a central nervous system depressant like alcohol is worlds apart from coming off a stimulant like cocaine. The risks are different, and the kind of support you'll need changes, too. To get a better handle on how substances are grouped, you can explore our guide to understanding drug addiction categories for successful recovery.
Let's break down what withdrawal typically looks like for some of the most common substance categories.
Alcohol Withdrawal Symptoms
Alcohol slows down your brain. To keep things running, your brain ramps up its own "excitatory" signals to compensate. When you suddenly take the alcohol away, that hyper-excited state is left unchecked, creating a cascade of withdrawal symptoms that can be intensely severe and even life-threatening.
Symptoms usually start to kick in within five to ten hours after the last drink. They often include:
- Physical Signs: Tremors (the "shakes"), heavy sweating, nausea, vomiting, headaches, a racing pulse, and high blood pressure.
- Psychological Signs: Overwhelming anxiety, irritability, insomnia, and intense nightmares.
In the most serious cases, a medical emergency known as delirium tremens (DTs) can develop, usually two to three days after the last drink. It’s marked by severe confusion, hallucinations, and dangerous shifts in breathing and circulation that require immediate medical intervention.
Opioid Withdrawal Symptoms
Opioids—like heroin, fentanyl, and prescription painkillers—work by attaching to special receptors in the brain. This floods your system with feel-good chemicals, creating a powerful sense of euphoria while blocking pain. When you stop, the body goes into a jarring rebound.
Withdrawal from opioids often feels like a brutal case of the flu. While it’s rarely life-threatening, it is profoundly uncomfortable. Symptoms typically begin within 12 to 30 hours and can include:
- Physical Signs: Deep muscle aches, stomach cramps, diarrhea, a runny nose, sweating, goosebumps, and dilated pupils.
- Psychological Signs: Agitation, anxiety, an inability to sleep, and relentless cravings.
Stimulant Withdrawal Symptoms
Stimulants like cocaine, methamphetamine, and prescription drugs like Adderall do the opposite of depressants—they put your central nervous system into overdrive. This produces a rush of energy, focus, and euphoria. Not surprisingly, the withdrawal that follows is often described as a deep "crash."
While you might not get the same kind of physical sickness you see with alcohol or opioids, the psychological fallout can be overwhelming and dangerous.
- Physical Signs: Crushing fatigue, a sharp increase in appetite, and slowed-down physical movements.
- Psychological Signs: Severe depression, intense irritability, apathy, paranoia, and powerful cravings. The risk of suicidal thoughts is very real during this period and needs to be taken seriously.
As you can see, the psychological toll is a major part of the experience, no matter the substance.
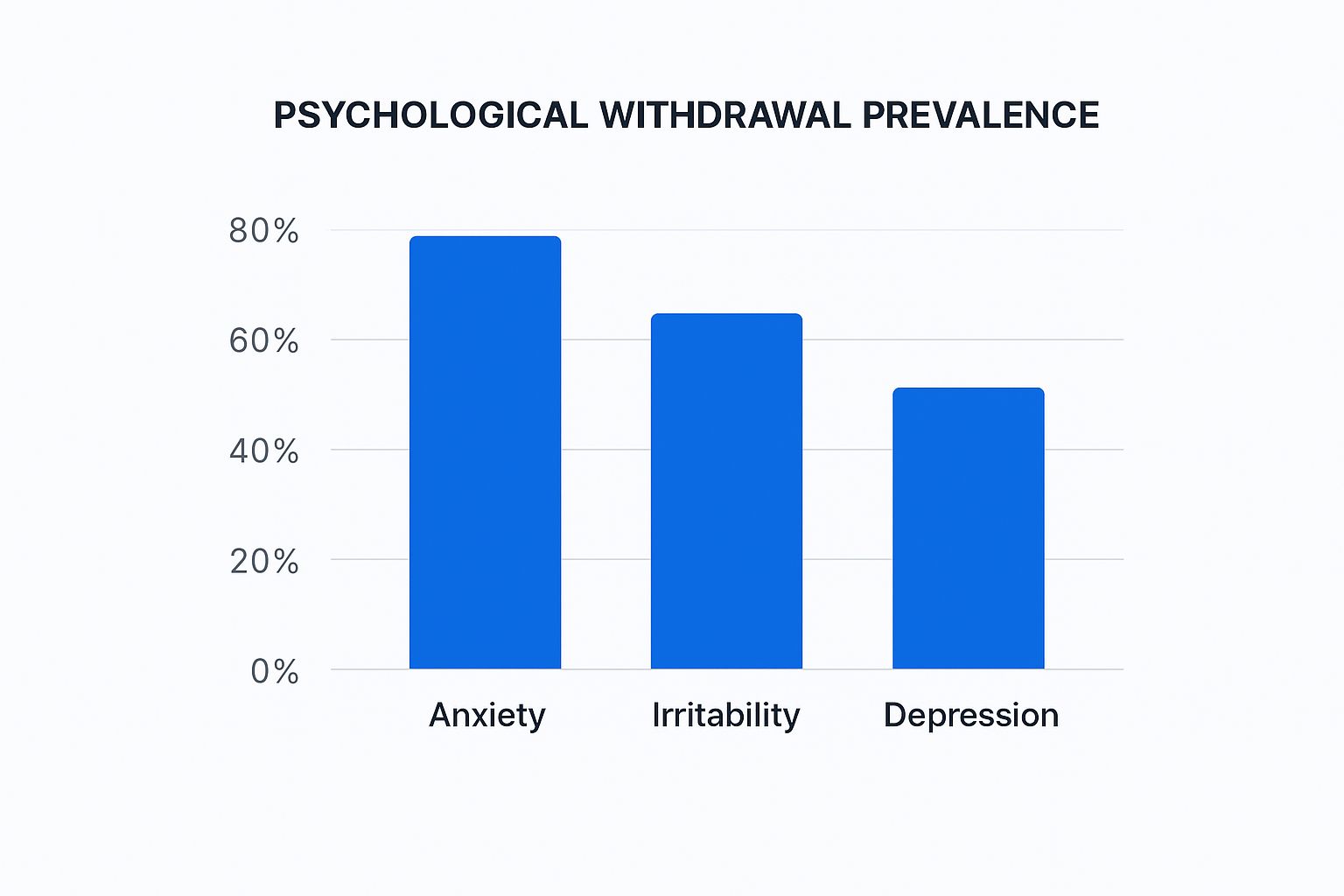
This data shows that emotional distress, especially anxiety, is an almost universal component of withdrawal.
A Comparative Look at Withdrawal Symptoms
To make these differences clearer, the table below compares the common symptoms across these major substance classes.
| Substance | Common Physical Symptoms | Common Psychological Symptoms |
|---|---|---|
| Alcohol | Tremors, sweating, nausea, vomiting, rapid pulse, seizures (in severe cases). | Intense anxiety, irritability, insomnia, confusion, hallucinations (in severe cases). |
| Opioids | Muscle aches, cramps, diarrhea, runny nose, sweating, goosebumps. | Agitation, anxiety, insomnia, strong cravings, yawning. |
| Stimulants | Extreme fatigue, increased appetite, slowed movements, physical agitation. | Severe depression, irritability, apathy, paranoia, intense cravings, suicidal thoughts. |
| Benzodiazepines | Tremors, sweating, muscle pain, increased heart rate, seizures (in severe cases). | Rebound anxiety, panic attacks, insomnia, sensory hypersensitivity. |
This side-by-side view really highlights how the physical risks from something like alcohol or benzodiazepine withdrawal differ from the profound psychological crash associated with stimulants.
Benzodiazepine Withdrawal Symptoms
Benzodiazepines, often called "benzos," are prescription sedatives like Xanax, Valium, and Klonopin. They're typically used for anxiety and insomnia and work in a way that's very similar to alcohol—by boosting the effects of GABA, a calming chemical in the brain. Because of this, withdrawal from benzos can also be dangerous and absolutely requires medical supervision.
The withdrawal journey for benzodiazepines can be long and complicated. Symptoms often come in waves, appearing, fading, and then returning over weeks or even months. Trying to navigate this without professional guidance is incredibly challenging.
Common symptoms you can expect include:
- Physical Signs: Increased heart rate, sweating, tremors, muscle pain, and, in severe cases, life-threatening seizures.
- Psychological Signs: A powerful return of anxiety (often called rebound anxiety), panic attacks, insomnia, and a heightened, almost painful, sensitivity to light and sound.
It’s clear that while things like anxiety and irritability are common threads running through most withdrawal experiences, the specific physical risks and the overall journey vary dramatically. This is exactly why a one-size-fits-all approach just doesn't work for detox.
How Long Do Withdrawal Symptoms Last?
When you’re preparing for recovery, one of the biggest questions is always, "How long will this last?" It's a fair question, but the answer isn't a single number. Think of withdrawal not as a quick sprint but as a journey with a few distinct stages. While everyone's path is unique, the general pattern is something we can anticipate.
The whole process really breaks down into two main phases. First, there's the acute phase—this is the intense, upfront part everyone thinks about. After that comes a much longer, quieter stage known as Post-Acute Withdrawal Syndrome (PAWS).
The Acute Phase: The Initial Peak
The acute phase is the storm before the calm. It kicks in shortly after you stop using a substance, and it’s your body's most intense, immediate reaction to not having it anymore. It's the peak of the mountain you have to climb first.
For most substances, this initial phase starts within hours of the last dose and can last anywhere from a few days to a couple of weeks.
- Onset: Symptoms might show up in as little as five to ten hours for alcohol, or within 12 to 30 hours for opioids.
- Peak: Things usually get the toughest around the 24 to 72-hour mark.
- Decline: After hitting that peak, the most severe symptoms thankfully start to fade over the next several days.
This is when the physical and psychological discomfort is at its absolute worst. It's also why medical supervision is so important during this window—it's all about staying safe and managing the most challenging symptoms. This isn't a small-scale problem, either. A global dataset tracking reports from 2004 to 2023 found over 94,000 instances of drug withdrawal syndrome across 79 countries, which really shows how common this intense initial phase is. You can dig into the data yourself in the full report from Frontiers in Pharmacology.
Post-Acute Withdrawal Syndrome: The Lingering Echoes
Once you’re through the storm of the acute phase, you might enter a much longer, more subtle stage called PAWS. If the acute phase was a hurricane, PAWS is the weeks of gray skies and scattered showers that follow. The intense physical sickness is gone, but you’re left with emotional and psychological ups and downs that can feel unpredictable.
PAWS involves less severe but persistent withdrawal symptoms that can last for weeks, months, or in some cases, even longer. This stage isn't about being physically ill; it’s about your brain slowly rewiring and finding its balance again.
Symptoms of PAWS often include:
- Mood swings and irritability
- Anxiety and depression
- Low energy and fatigue
- Trouble sleeping
- Brain fog or difficulty concentrating
These symptoms tend to come and go in waves, which can be incredibly frustrating. Knowing about PAWS is crucial, though, because it helps make sense of why you might still feel "off" long after detox is over. Recognizing that these feelings are a normal part of your brain healing is a massive step in preventing relapse. To get a better handle on this part of the journey, our guide on understanding the stages of the recovery process is a great resource.
At the end of the day, any timeline is just an estimate. The substance you used, how long you used it, and your own personal health are all going to shape what your withdrawal experience looks and feels like.
What Shapes Your Withdrawal Experience?
Ever wonder why one person can ditch their daily coffee with just a mild headache, while someone else trying to quit alcohol faces a life-threatening emergency? The intensity of withdrawal is far from random. It's a complex interplay of several key factors.
Think of it less as a test of willpower and more as a predictable outcome of your unique biology, your history with the substance, and the substance's own chemical properties.
The Drug Itself and Your History With It
The most significant factor, hands down, is the substance you've been using. Different drugs hijack the brain in different ways, which means they have very different withdrawal patterns. Kicking a stimulant habit, for instance, often leads to a brutal psychological crash, whereas stopping long-term alcohol use can trigger dangerous physical symptoms, including seizures.
But it’s not just about what you used; it’s about how you used it. Your personal history with the substance is a huge piece of the puzzle. Key elements include:
- How long you've been using: Someone with a decade of heavy drinking under their belt is going to have a much rougher road than someone who's been drinking heavily for six months. Time builds deeper dependence.
- How much you were taking: Higher doses lead to a more significant physical dependence. Your brain has to work much harder to recalibrate, making the withdrawal that much more intense.
- How often you used: Daily use creates a constant state of dependence that your body comes to expect. When that substance is suddenly gone, the shock to your system is far greater than it would be for an occasional user.
Your Personal Health and Well-being
Your body is the stage where all of this plays out, and your overall health has a massive impact. Your age, metabolism, and any underlying medical issues—especially problems with your heart or liver—can seriously complicate withdrawal and make symptoms harder to manage.
Your mental state is just as crucial. If you're already navigating anxiety, depression, or PTSD, withdrawal can feel like pouring gasoline on a fire. It often magnifies these existing symptoms, trapping you in a vicious cycle where the psychological pain of withdrawal makes your mental health condition worse, which in turn makes the withdrawal feel even more unbearable.
Think of it this way: the withdrawal experience is the body's "snap-back" effect. The longer and more intensely you've used a substance, the further your body has stretched to adapt. The snap-back will naturally be more severe and last longer.
How You Decide to Quit
Finally, the way you stop using can make all the difference in the world.
Going "cold turkey" means stopping all at once. This approach can throw your system into a state of shock, triggering the most extreme and dangerous withdrawal symptoms. It's like ripping a bandage off a deep wound.
A much safer, more manageable path is tapering. This means gradually decreasing your dose over time, almost always with a doctor's guidance. Tapering gives your brain and body the time they need to gently readjust their chemistry, which dramatically softens the blow of withdrawal. For substances like alcohol and benzodiazepines, this isn't just a suggestion—it can be a life-saving necessity, as quitting cold turkey can be fatal.
When You Absolutely Need Medical Help

The thought of going through withdrawal is scary enough on its own. But it's absolutely critical to understand the line between intensely uncomfortable and genuinely life-threatening. The reality is, not all withdrawal is created equal. For some substances, trying to go it alone isn't just a bad idea—it can be fatal.
Let's use an analogy. Withdrawing from opioids or stimulants is like weathering a brutal hurricane. It's awful, but you can usually get through it. But withdrawing from alcohol or benzodiazepines? That’s like trying to land a plane in that hurricane after the pilot has passed out. Your body's core systems are at risk of failing.
Recognizing Red-Flag Symptoms
Some symptoms are more than just a rough patch; they are blaring red flags of a medical crisis. If you or someone you're with experiences any of these, call 911 or head to an emergency room immediately. There’s no time to wait.
These are non-negotiable emergencies:
- Seizures: Any uncontrolled shaking or convulsions signal dangerous overactivity in the brain.
- Hallucinations: Seeing or hearing things that aren't there is a sign of a severe neurological breakdown.
- Extreme Confusion or Disorientation: Not knowing where you are, who people are, or what's happening is a major warning.
- Delirium Tremens (DTs): This is a severe, life-threatening state from alcohol withdrawal, bringing on intense confusion, fever, agitation, and a dangerously fast heart rate. It usually kicks in two to three days after the last drink.
Trying to "tough it out" at home with these symptoms can cause permanent damage or even death. This is precisely when professional medical help is not just an option, but a necessity.
The Dangers of Certain Substances
So, why are some substances so much more dangerous to quit? It all comes down to how they mess with your brain's fundamental operating system.
Alcohol and benzodiazepines (like Xanax and Valium) are central nervous system depressants. Over time, your brain compensates for their slowing effect by ramping up its own electrical activity just to keep things running normally. When you suddenly take the substance away, the brain doesn't get the memo—it stays in that hyper-excited, over-amped state. This is what can trigger seizures, heart failure, and stroke.
This is exactly why quitting "cold turkey" from these drugs without a doctor's supervision is so incredibly risky.
The Benefits of Medically Supervised Detox
Deciding on a medically supervised detox isn't about being weak; it's about being smart and safe. The advantages are real and can be the deciding factor between relapse and a successful recovery.
- Safety First: In a medical setting, your vitals are monitored 24/7. If dangerous symptoms like a seizure start, a team is right there to intervene.
- Symptom Management: Doctors can use FDA-approved medications to calm the storm, easing the worst of the physical and psychological pain and making the whole process more manageable.
- Stable Foundation: Getting through detox safely gives you a solid, healthy footing for the real work of recovery. Many find that a structured program, like an inpatient alcohol rehab, provides the support needed to build a new life.
- Nutritional Support: Long-term substance use wreaks havoc on your body's nutrition, which makes withdrawal even worse. A medical team can restore what's been lost with IV fluids and essential vitamins.
Getting through withdrawal safely is the first, most crucial step. Knowing the signs that scream for help gives you the power to protect yourself—or someone you love—from a preventable tragedy.
A Few Final Thoughts on Getting Through Withdrawal
We've covered a lot of ground here—the science, the symptoms, and the timelines. It can feel like a lot to take in, so let's boil it all down to the essentials. Think of these as the core truths to hold onto as you or a loved one navigate this process.
Arming yourself with the right information is one of the most powerful things you can do.
At its heart, withdrawal is a completely natural, if difficult, medical event. It's simply your body’s way of recalibrating after becoming dependent on a substance. Seeing it this way helps reframe the experience: it’s not a moral failing, but a biological hurdle on the path to getting well.
Frequently Asked Questions About Withdrawal

When you're facing withdrawal, questions and uncertainties are completely normal. Let’s clear up some of the most common concerns people have as they navigate this challenging but critical phase of recovery.
Can you go through withdrawal from prescribed medications?
Yes, absolutely. It's a common misconception that withdrawal only happens with illegal drugs or alcohol. Your body can become physically dependent on many prescription medications after long-term use, especially things like opioids, benzodiazepines, and even some antidepressants.
Take antidepressants, for example. For people who have used them for a while, stopping suddenly can be a real shock to the system. In fact, research from the UBC Therapeutics Initiative shows that up to 60% of patients experience symptoms like dizziness, nausea, and vertigo when they stop. This is precisely why doctors insist on tapering off these medications slowly.
Is it safe to detox at home?
This is probably one of the most important questions you can ask, and the answer isn't always straightforward. While detoxing in the comfort of your own home might sound appealing, for some substances, it's incredibly dangerous.
When it comes to alcohol and benzodiazepines, detoxing at home is never a safe bet. The withdrawal from these substances can trigger life-threatening complications, including seizures or delirium tremens. A medically supervised detox is the only way to manage these risks safely.
For other substances, whether at-home detox is an option really depends on your health, how long you were using, and what you were using. The golden rule? Always talk to a doctor or addiction specialist first.
Does everyone experience Post-Acute Withdrawal Syndrome (PAWS)?
Not everyone goes through Post-Acute Withdrawal Syndrome (PAWS), but it’s more common than you might think. Whether you experience it often depends on the substance you were using and for how long.
PAWS can be frustrating because the symptoms—like intense mood swings, fatigue, or anxiety—tend to come and go in waves, sometimes long after the acute detox phase is over. It helps to remember that this is just your brain’s way of healing and rebalancing itself. Understanding that these lingering effects are a part of the process can give you the strength to stay on track with your recovery.
What is the fastest way to get through withdrawal?
While it's natural to want the process to be over quickly, there are no safe shortcuts for withdrawal. The "fastest" way is often the most dangerous, like quitting "cold turkey." The safest and most effective approach is a medically supervised detox where professionals can use medications to manage your symptoms, making the experience more bearable. This approach prioritizes your health and sets a stronger foundation for long-term recovery over a risky, rapid detox.
Getting through withdrawal is a massive first step on the road to a new life. At StartDrugRehab.com, our goal is to connect you with the resources and professional care you need to make that journey a successful one. If you or someone you care about needs support, visit us at https://startdrugrehab.com to explore your options.

