At first glance, Suboxone and Subutex seem almost identical. The critical difference, however, lies in a single ingredient that fundamentally changes how each medication is used in opioid addiction treatment.
While both drugs rely on buprenorphine to ease withdrawal and curb cravings, Suboxone has an added component: naloxone. This addition is a safety measure designed to prevent misuse. Subutex, which contains only buprenorphine, is typically reserved for specific, highly supervised clinical settings.
Key Takeaways
- Core Difference is Naloxone: Suboxone contains both buprenorphine and naloxone, while Subutex contains only buprenorphine. The naloxone is a misuse deterrent.
- Different Clinical Roles: Subutex is primarily used for the initial, supervised phase of treatment (induction) and for specific populations like pregnant patients.
- Suboxone for Maintenance: Suboxone is the standard for long-term, outpatient maintenance therapy due to its added safety feature against intravenous misuse.
- Equal Efficacy: When taken as prescribed, both medications are equally effective at managing opioid withdrawal symptoms and cravings, as the therapeutic effect comes from the shared active ingredient, buprenorphine.
Understanding the Core Composition

To really grasp the Suboxone vs. Subutex comparison, you have to look at their active ingredients. This is where they part ways. Both are cornerstones of medication-assisted treatment (MAT) for opioid use disorder, but their formulations are tailored for different phases and scenarios in a person's recovery.
The therapeutic engine in both is buprenorphine, a partial opioid agonist. Imagine it as a key that fits into the brain's opioid receptors but only turns part of the way. It’s just enough to stop withdrawal and satisfy cravings, but not enough to produce the intense high associated with full agonists like heroin or oxycodone. This stabilizing effect is what allows patients to step away from the chaos of addiction and engage with their recovery.
The Role of Naloxone
Suboxone's formula introduces a second active ingredient: naloxone. An opioid antagonist, naloxone's job is to block opioid receptors, and it's the defining difference between these two medications.
The naloxone in Suboxone is a clever safety mechanism. When you take the medication as prescribed—dissolving it under your tongue—the naloxone isn't absorbed well and remains dormant. But if someone tries to inject the medication to get high, the naloxone activates instantly, blocking all opioid effects and throwing the person into immediate, severe withdrawal.
This built-in deterrent is why Suboxone is the standard choice for long-term, outpatient treatment where the potential for misuse is a greater concern. While both are effective tools, their unique compositions are meant for different clinical needs. You can learn more about the buprenorphine market and its role in addiction treatment for a broader perspective.
Suboxone vs Subutex at a Glance
For a quick summary of the key distinctions, the table below provides a clear, side-by-side view.
| Feature | Suboxone | Subutex |
|---|---|---|
| Active Ingredients | Buprenorphine & Naloxone | Buprenorphine Only |
| Primary Purpose | Long-term maintenance | Medically supervised induction, specific populations |
| Misuse Deterrent | Yes (Naloxone) | No |
| Common Form | Sublingual film or tablet | Sublingual tablet |
This table highlights the fundamental trade-offs. Suboxone offers an added layer of safety against misuse, making it suitable for broader use, while Subutex provides a simpler formulation for controlled environments or patients with specific sensitivities.
How Each Medication Works in the Body
To really get to the heart of the Suboxone vs. Subutex debate, we need to look at what happens inside the body when someone takes them. At their core, both medications are built around the same active ingredient: buprenorphine. This is the workhorse component doing the heavy lifting in treating opioid use disorder.
Buprenorphine is what we call a partial opioid agonist. It's a bit different from full agonists like heroin or oxycodone. Instead of flipping the opioid receptors in the brain all the way "on," think of buprenorphine as setting them to a "dim" position. It binds to those receptors just enough to keep cravings and withdrawal at bay, but without producing the intense high that full opioids do.
This creates a "ceiling effect," which is a crucial safety feature. After a certain dose, taking more buprenorphine doesn't increase the opioid effects. This dramatically lowers the risk of respiratory depression, the primary cause of fatal opioid overdoses, making it a much safer long-term treatment option.
The Naloxone Difference in Action
So, if both have buprenorphine, what's the big deal? The difference is naloxone, which is added to Suboxone but not Subutex. Naloxone is a pure opioid antagonist—its only job is to block opioid receptors and reverse the effects of opioids.
When you take Suboxone as directed by dissolving it under your tongue, the naloxone component is poorly absorbed. Almost none of it makes it into your bloodstream, so it remains inactive. The buprenorphine gets to work as intended, and the patient gets the therapeutic relief they need.
But the game changes entirely if someone tries to misuse it.
If a person attempts to dissolve Suboxone and inject it, the naloxone is absorbed instantly and completely. It rushes to the brain's opioid receptors, kicking the buprenorphine off and blocking them entirely. This action triggers immediate and severe withdrawal symptoms, a highly unpleasant experience known as precipitated withdrawal. It's a powerful, built-in deterrent against intravenous abuse.
This is why the route of administration is so critical.
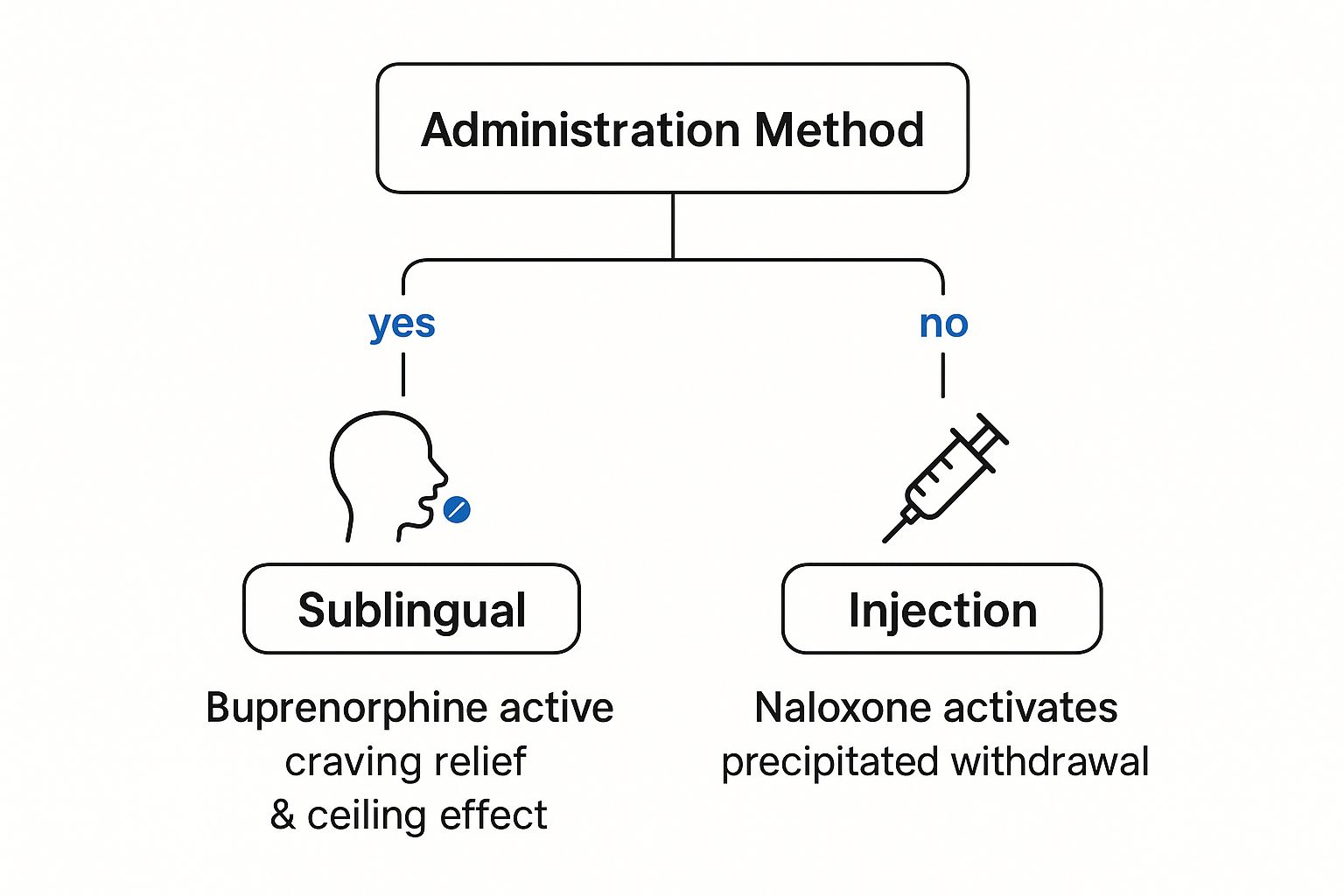
As you can see, using the medication sublingually leads to the intended therapeutic effect. Trying to inject it, however, unleashes the naloxone and its deterrent effects. This clever pharmacological design is precisely why Suboxone is the go-to choice for most outpatient treatment plans, where the potential for misuse or diversion is a greater concern. To understand more about this reaction, it's helpful to learn about what are withdrawal symptoms and their underlying mechanisms.
Ultimately, this fundamental difference in their formulation is what guides a clinician's decision on which medication is the right fit for a patient's specific situation.
Matching the Right Medication to the Patient

When it comes to Suboxone versus Subutex, there’s no simple "better" option. The real question is, which medication is right for this patient, right now? Clinicians make this call by carefully looking at the patient's stage of treatment, their living situation, and any specific medical needs. Ultimately, the core difference between Suboxone and Subutex is what allows for such personalized care.
This careful decision-making is most critical at the very beginning of treatment—the induction phase. In this medically supervised setting, the absolute priority is getting the patient stable safely and quickly.
The Role of Subutex in Supervised Settings
During the induction phase, clinicians often lean on Subutex. Since it contains only buprenorphine, it allows them to focus purely on stabilizing the patient without the added variable of naloxone. This keeps things straightforward, zeroing in on managing withdrawal and cravings in a controlled, secure environment.
Subutex also happens to be the standard of care for one very specific group: pregnant patients.
While naloxone isn't known to be harmful during pregnancy, the guiding principle in medicine is to minimize any unnecessary medication exposure for the fetus. Buprenorphine on its own is proven to be safe and effective, so Subutex (or its generic form) becomes the go-to choice to protect the health of both parent and child.
This specific use case really underscores how individual patient factors drive the treatment plan. Once a patient is stabilized and ready for a less supervised recovery setting, the plan often shifts.
Suboxone for Long-Term Maintenance and Safety
For long-term, outpatient treatment, the conversation almost always turns to Suboxone. As patients take on more responsibility for their recovery outside the clinic walls, the potential for medication misuse or diversion becomes a bigger concern. This is exactly where Suboxone’s unique formulation shines.
The naloxone component is designed specifically to deter misuse, adding a crucial layer of safety that supports a person's recovery journey for the long haul. This feature makes it the preferred choice for the vast majority of people in ongoing medication-assisted treatment (MAT).
In many cases, moving from one medication to the other is a standard, planned part of the recovery roadmap.
- Induction Phase: Treatment often begins with Subutex in a closely monitored setting to achieve stability.
- Maintenance Phase: Patients usually transition to Suboxone for its built-in safety features in an outpatient environment.
- Special Populations: Subutex remains the clear choice for pregnant patients or individuals with a rare allergy to naloxone.
This thoughtful, situational approach ensures every person gets the right support on their unique path forward.
Comparing Safety, Efficacy, and Side Effects
People often ask, "Which one is safer? Which one works better?" It's a fair question, but the answer isn't a simple one-or-the-other. Because Suboxone and Subutex share the same primary active ingredient—buprenorphine—they are remarkably similar in both effectiveness and their potential side effects.
When taken exactly as a doctor prescribes, both are incredibly effective tools for managing opioid cravings and keeping the harsh symptoms of withdrawal at bay. The real therapeutic heavy lifting is done by buprenorphine, so patients generally get the same level of craving control from either medication.
Common Side Effects and Risks
The side effects for both medications are also nearly identical, as they stem directly from the buprenorphine. As a patient’s body gets used to the treatment, these often become less intense or go away completely.
Some of the most common ones include:
- Nausea and vomiting
- Headaches
- Constipation
- Feeling drowsy or, conversely, having trouble sleeping (insomnia)
- Sweating
While these are typically manageable, always keep your doctor in the loop. It’s a common misconception that the naloxone in Suboxone causes side effects when taken correctly under the tongue; it's barely absorbed that way. It's also critical to consider other medications. For instance, knowing the details of Klonopin uses and side effects is crucial if a doctor prescribes it alongside your treatment.
The single biggest risk with both Suboxone and Subutex is something called precipitated withdrawal. This isn't your typical withdrawal; it's a sudden, intense, and immediate onset of severe withdrawal symptoms.
This happens if you take either medication too soon, while full agonist opioids like heroin or fentanyl are still attached to the opioid receptors in your brain. To prevent this, doctors are extremely careful about timing the first dose, waiting until a patient is already in a mild to moderate state of withdrawal. This induction process is fundamental to starting treatment safely.
A Closer Look at Precipitated Withdrawal
While both medications carry this risk, the way it can happen differs slightly, especially when misuse is involved. If someone were to inject Suboxone while other opioids are in their system, the naloxone would activate instantly. It would aggressively rip the other opioids off the brain's receptors, triggering a particularly brutal withdrawal.
When taken properly under the tongue, however, the naloxone stays dormant, and the risk is virtually the same as with Subutex. In the end, a doctor’s choice between Suboxone and Subutex isn't usually about which one is "better" or "safer" in general. It's about the individual patient, their specific situation, and their potential risk for misuse.
Cost, Availability, and Insurance Coverage

While the clinical differences between Suboxone and Subutex are important, the practical side of things—cost, what your insurance will cover, and what the pharmacy has in stock—often dictates which medication a patient actually receives. These real-world factors can be just as influential as the pharmacology.
At one time, brand-name Suboxone dominated the market. That's no longer the case. The landscape completely shifted once generic versions of both medications became available. Now you can get generic buprenorphine (the equivalent of Subutex) and generic buprenorphine/naloxone (the equivalent of Suboxone), and this has been a total game-changer for accessibility and affordability.
Insurance and Market Dynamics
Most insurance plans, including Medicaid and Medicare, provide solid coverage for buprenorphine-based medications. They're considered essential for treating opioid use disorder, so insurers are on board, though they almost always push for the more affordable generic options.
This widespread availability of generics has been crucial for getting more people into treatment. It's torn down one of the biggest barriers to recovery—cost—allowing countless individuals to access these life-saving medications.
The numbers back this up. The global Suboxone market was valued at USD 6,163.9 million back in 2022 and is expected to keep growing, largely thanks to these generic approvals. A huge milestone was the FDA's 2020 approval of a generic buprenorphine and naloxone tablet, which made treatment significantly more attainable. You can discover more about the Suboxone market growth and how it impacts patient access.
In the end, while your doctor determines the best clinical fit, your insurance plan's formulary and what your local pharmacy carries will likely influence whether you walk out with a brand-name or generic version of either medication.
Making the Right Treatment Choice
Deciding between Suboxone and Subutex is a serious conversation to have with your doctor. While this guide gives you the background, the final call always comes down to a team decision that fits your unique recovery needs. The more you understand the core differences, the better prepared you'll be for that talk.
Ultimately, the best medication is the one that fits your medical situation and helps you meet your long-term recovery goals. This decision is often influenced by where you're receiving care—for instance, a supervised medical setting versus a take-home prescription. You can learn more about how the environment shapes treatment by exploring the differences between inpatient vs outpatient rehab.
What to Discuss With Your Doctor
To get the most out of your appointment, it helps to go in with a few key points straight. These four distinctions get to the heart of the difference between Suboxone and Subutex and how they’re used in treatment.
Knowing these fundamentals empowers you to be an active partner in creating your treatment plan. The real goal is finding the option that offers the most stability and safety for your specific journey.
-
The Naloxone Difference: The only thing separating these two medications is that Suboxone contains naloxone. It's added purely as a safety measure to discourage misuse and has no effect when the medication is taken as directed.
-
Subutex is for Specific Cases: Subutex is almost always reserved for two situations: the very beginning of treatment under close medical supervision (the induction phase) and for patients who are pregnant.
-
Suboxone is for the Long Haul: Once a patient is stable, Suboxone becomes the go-to for long-term maintenance treatment. Its built-in safety features make it the standard for outpatient care where the risk of misuse is higher.
-
Both are Equally Effective: When used correctly, both medications are just as good at stopping cravings and withdrawal symptoms. That’s because the real therapeutic work is done by the buprenorphine, which is the active ingredient in both.
The demand for these treatments is incredibly high. North America alone makes up 45.1% of the global buprenorphine market, driven by the ongoing opioid crisis and government support for effective treatments. You can dig deeper into the Opioid Use Disorder Market to see the bigger picture.
Frequently Asked Questions (FAQ)
When you're exploring treatment for opioid use disorder, you’re bound to have a lot of questions. That’s a good thing. Getting clear on the details helps you take an active role in your recovery. Here, we'll tackle some of the most common questions people ask about Suboxone and Subutex.
What is the main difference between Suboxone and Subutex?
The single biggest difference is an ingredient called naloxone. Suboxone contains both buprenorphine and naloxone. Subutex contains only buprenorphine. The naloxone is added to Suboxone to deter misuse; it causes immediate withdrawal symptoms if the medication is injected, but remains inactive when taken correctly under the tongue.
Can I switch from Subutex to Suboxone?
Yes, and it’s very common. Many treatment plans start with Subutex in a medically supervised setting to stabilize a patient. Once the patient is stable, their doctor will often switch them to Suboxone for long-term maintenance treatment due to its lower potential for misuse in an outpatient setting.
Why is Subutex used during pregnancy instead of Suboxone?
Medical guidelines prioritize minimizing a fetus's exposure to medications. While naloxone (the extra ingredient in Suboxone) is not considered harmful, buprenorphine alone (Subutex) has a well-established safety record for use during pregnancy. To be as safe as possible, Subutex is the standard of care for pregnant patients.
Does one work better for cravings than the other?
No. When taken as prescribed, both medications are equally effective at controlling cravings and withdrawal symptoms. The therapeutic effect comes from buprenorphine, which is the primary active ingredient in both drugs. The choice between them is based on safety considerations and the patient's specific clinical situation, not on one being "stronger" than the other.
Is Suboxone more expensive than Subutex?
Previously, brand-name Suboxone was more expensive. However, with the availability of generic versions for both medications, the cost difference is now minimal. Your out-of-pocket cost will depend more on your insurance coverage and whether you receive a brand-name or generic drug. Most insurance plans prefer the more cost-effective generic options.
Finding the right path to recovery begins with having the right information. At StartDrugRehab.com, we provide the resources and support you need to make confident decisions about your treatment. Explore our expert guides and connect with trusted providers by visiting https://startdrugrehab.com.

