The first real step toward recovery isn't a dramatic, movie-like scene. It rarely is. More often, it's a quiet, nagging feeling that grows over time—a personal realization that something has to give.
It's about finally admitting to yourself that the way things are isn't working anymore. Recognizing this isn't a sign of weakness. It's an act of profound courage and the true beginning of your journey back to yourself.
Key Takeaways
- Self-Awareness is the First Step: Recognizing the subtle signs that your substance use is negatively impacting your life is the true beginning of the recovery journey. This internal admission is an act of strength, not weakness.
- Professional Detox is a Medical Necessity: Never attempt to detox from substances like alcohol or benzodiazepines alone. Medically supervised detox is crucial for safely managing potentially life-threatening withdrawal symptoms.
- Treatment Must Fit Your Life: There is no one-size-fits-all recovery plan. Choosing between inpatient, PHP, or IOP depends on your specific needs, the severity of the addiction, and your daily responsibilities.
- Community is Crucial for Long-Term Success: Addiction thrives in isolation, while recovery happens in community. Building a strong support system through peer groups, sponsors, and family therapy is essential for lasting change.
Acknowledging It's Time for a Change

The path to recovery often starts with a subtle, persistent feeling that something is fundamentally wrong. This internal shift is the most important step you’ll ever take.
Confronting this feeling is tough. It might show up as a constant sense of unease or the slow realization that your world is shrinking to make room for your substance use. So many people I've worked with started to notice these signs long before any major crisis forced their hand.
Recognizing the Subtle Signs
The real indicators that you might need help are usually woven right into your daily life. They’re the small compromises you make and the little adjustments you barely notice, but over time, they paint a much bigger picture.
Think about it. Do any of these sound familiar?
- That nightly glass of wine has gone from a choice to a non-negotiable ritual you need just to feel normal.
- You start dodging social events where you know you won't be able to use your substance of choice.
- Your go-to justifications—"I've had a hard week" or "I'm just having fun"—are starting to sound hollow, even to your own ears.
- You've tried to cut back on your own, only to find yourself right back in the same patterns within a few days or weeks.
Recognizing these patterns isn't about shame or blame. It’s about honesty. It's an act of self-awareness that gives you the power to finally do something about it.
This initial awareness is a common starting point. In fact, the first steps to recovery in mental health often begin with simply understanding you're not alone. As of 2025, over one billion people worldwide are living with mental health disorders, which cost the global economy about $1 trillion annually in lost productivity. It's a massive, shared human experience.
The Courage to Ask for Help
Making the decision to get help is a true act of strength, not a confession of failure. It’s the moment you decide to take back the controls. This is a deeply personal choice, and it takes real guts.
This process of self-reflection is what builds the internal drive you need to make a lasting change. It can be helpful to start exploring different therapeutic approaches early on. For example, learning about what is motivational interviewing can show you how therapists help people find their own reasons to change. It’s a powerful approach that respects your independence while guiding you toward a healthier life.
Getting Through Detox: Your Safe and Supported First Step
Let’s be honest—the thought of detox can be terrifying. It's often the biggest, most daunting hurdle you feel you have to clear before recovery can even begin. You're not just fighting a craving; your body is physically reacting to the absence of a substance it has learned to rely on.
This initial phase is all about managing withdrawal. Whether you’re coming off alcohol, opioids, or something else, your body has to readjust. The symptoms and how intense they get can be wildly different for everyone, which is exactly why a cookie-cutter approach is a recipe for failure. For most people, getting this part right is the most critical of the first steps to recovery.
Why You Shouldn't Go It Alone
Trying to detox cold turkey, especially from substances like alcohol or benzodiazepines, is more than just uncomfortable—it can be life-threatening. The risk of severe medical complications, including seizures or delirium tremens (DTs), is very real. This is why professional medical supervision isn’t just a good idea; it’s a must.
Doctors and nurses can provide medications to make you more comfortable, keep a close watch on your vitals, and step in immediately if something goes wrong. You can get a better sense of what withdrawal symptoms are and why they need to be handled with care. This professional oversight makes sure you get stable safely, giving you a solid foundation for everything that comes next.
Detoxing isn't a test of willpower. It's a medical event. The single best decision you can make for your health right now is to treat it that way and get professional help.
Finding the Right Detox Setting for You
The best place for you to detox will depend on your unique situation—what substance you used, for how long, and your overall physical health.
- Medically Supervised Inpatient Detox: Think of this as 24/7 medical care in a live-in facility. It's the safest bet for anyone with a severe dependency, especially on alcohol or benzos. You have round-the-clock monitoring and medical staff ready to act instantly if needed.
- Structured Outpatient Programs: If your dependency is less severe and you have a solid, stable home life, an outpatient program could work. You'll go to a clinic for regular check-ins but continue living at home, which lets you keep up with work or family duties.
For instance, a person who has been drinking heavily for years will almost certainly need the safety of an inpatient facility to manage dangerous withdrawal symptoms. On the flip side, someone with a more recent, milder dependency might do just fine with an outpatient plan, as long as they have a great support system at home.
The infographic below shows just how much the setting matters when it comes to complication rates and how long detox should last. It really brings home the risks of trying to do it without support.
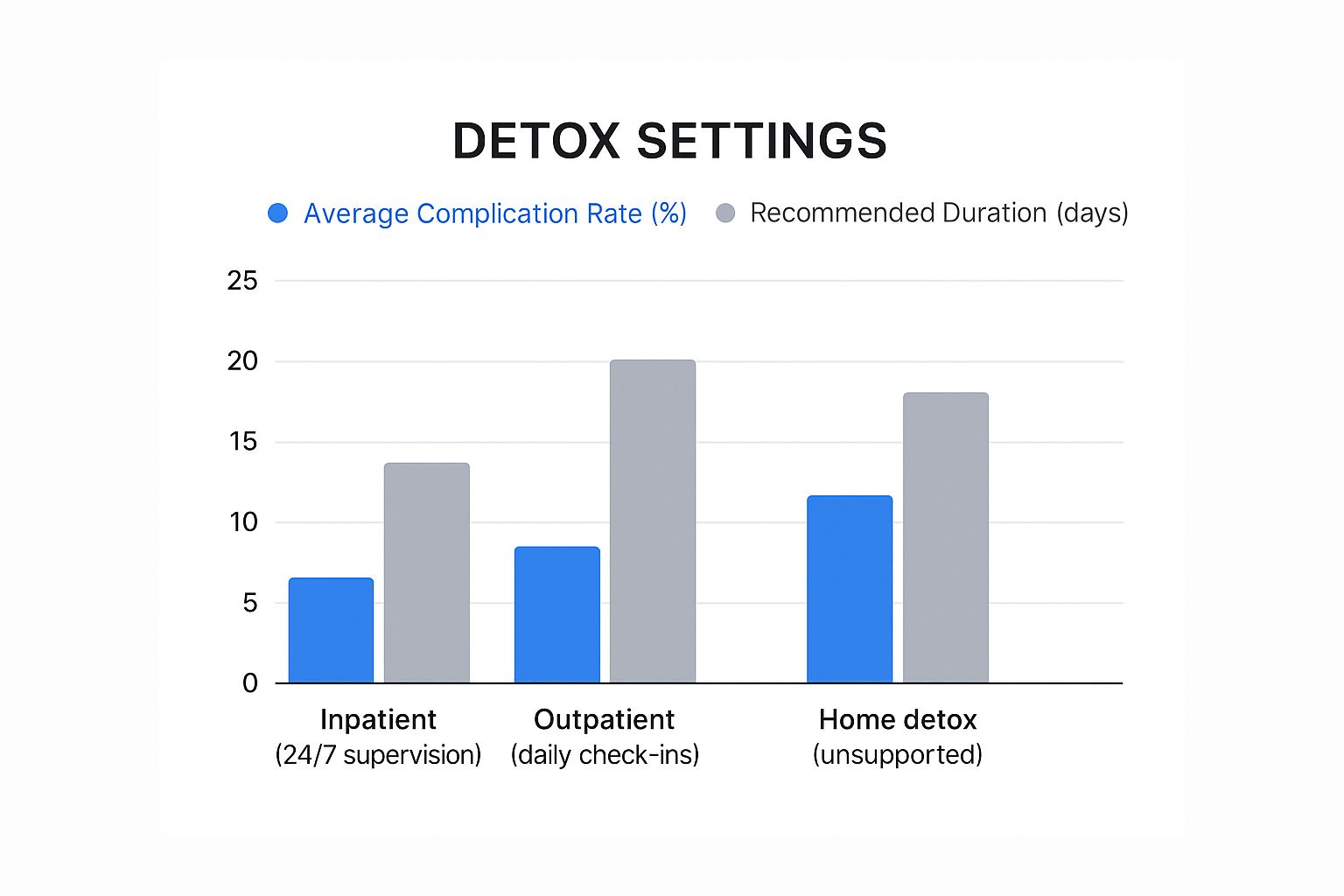
The numbers don't lie. Professional supervision dramatically lowers the risk of something going wrong, paving a much safer road forward. This isn't about choosing what's convenient; it's about choosing what gives you the best odds of a successful start.
Finding a Treatment Path That Fits Your Life

Once you’re through detox, the next big decision is figuring out which kind of treatment program actually works for you. There's no magic bullet here. The best path is the one that fits your real-world responsibilities, personal needs, and where you're at with your addiction. Making this choice is one of the most powerful first steps to recovery you can take.
Feeling confident in that decision starts with knowing what's out there. The good news is that addiction treatment has come a long way, and your options are broader and more flexible than ever before.
Just think about it: over the last 75 years, our approach to mental health and addiction has changed dramatically. What started with the introduction of new medications in the 1950s has grown to include a whole spectrum of evidence-based therapies and recovery models. NAMI has some great information on these milestones if you're curious about the history.
Exploring Your Treatment Options
The core difference between programs comes down to structure and intensity. You're looking for that sweet spot—the right amount of support to keep you safe and moving forward, but with enough independence to start rebuilding your life.
Let’s break down the most common levels of care you'll encounter.
-
Inpatient or Residential Rehab: This is the most immersive and structured choice. You live right at the facility, getting 24/7 medical supervision and therapeutic support. It's designed to pull you completely out of your daily environment and away from triggers.
-
Partial Hospitalization Program (PHP): Think of this as a step down from inpatient. You'll spend a significant part of your day in treatment, usually five to seven days a week, but you head home or to a sober living house at night.
-
Intensive Outpatient Program (IOP): IOPs offer even more flexibility. Treatment sessions typically run for a few hours a day, maybe three to five days a week. This structure is often a good fit if you need to keep up with work, school, or family life while still getting solid, consistent support.
Your choice of treatment isn’t a lifelong commitment to one specific level of care. It’s about finding the right starting point. Many people step down through these levels as they grow stronger in their recovery.
How Different Programs Stack Up
Choosing the right level of care can feel overwhelming, but laying out the options side-by-side often makes the decision clearer. It all comes down to what you need right now.
Here's a quick comparison to help you see how these programs differ and who they're best suited for.
Comparing Addiction Treatment Options
| Treatment Type | Intensity & Time Commitment | Ideal Candidate | Key Focus |
|---|---|---|---|
| Inpatient/Residential | 24/7 care for 30-90 days. | Someone with severe addiction, co-occurring disorders, or an unstable home environment. | Medical stabilization, intensive therapy, and building a foundation in a trigger-free setting. |
| Partial Hospitalization (PHP) | 5-8 hours/day, 5-7 days/week. | Someone who needs more support than outpatient but has a stable living situation. | Structured daily therapy and skill-building while transitioning back to daily life. |
| Intensive Outpatient (IOP) | 3-4 hours/day, 3-5 days/week. | Someone with a strong support system and the ability to manage daily responsibilities. | Integrating recovery skills into real-world scenarios like work, school, and family. |
Looking at this table, you can start to see which path might align best with your current life circumstances and recovery goals. Remember, the goal is progress, not perfection.
The Role of Therapy in Building a New Life
No matter which door you walk through—inpatient, PHP, or IOP—therapy will be the engine of your recovery. This is where you do the real work. It’s where you'll start to untangle the roots of your addiction and learn new, healthier ways to handle whatever life throws at you.
One of the most powerful tools you'll likely encounter is Cognitive Behavioral Therapy (CBT). It’s a practical, hands-on approach that helps you spot the negative thoughts and automatic behaviors that kept you stuck.
For instance, maybe stress is a major trigger for you. Instead of that automatic impulse to use, CBT gives you the skills to pause, recognize the feeling for what it is, and make a different choice—like calling a supportive friend, going for a run, or just stepping outside for some fresh air. It's about building a whole new playbook for your life.
Making an informed choice is so much easier when you can really dig into the details. Our guide on inpatient vs. outpatient rehab breaks things down even further to help you weigh the pros and cons for your unique situation. Choosing the right path is a huge step toward building a sober life that you genuinely love.
Building Your Personal Recovery Community

If there’s one profound truth I’ve seen in recovery, it’s this: you can’t do it alone. Addiction absolutely thrives in isolation, but healing happens when we connect with others. Building a network of people who actually understand and champion your journey is one of the most powerful first steps to recovery you will ever take.
This goes way beyond just having a list of names to call when you're struggling. It's about consciously weaving a new social fabric for your life—one that reinforces sobriety, encourages raw honesty, and genuinely celebrates your wins, no matter how small. You’re intentionally picking your team.
Finding Your People in Peer Support Groups
Peer support groups offer something invaluable that even the most well-meaning family member can't: a truly shared experience. Walking into a room full of people who just get it without you having to say a word is an incredibly powerful feeling.
There are several great options out there, each with a slightly different flavor:
- 12-Step Programs: Groups like Alcoholics Anonymous (AA) and Narcotics Anonymous (NA) offer a structured, spiritual framework for recovery. The core of these programs is peer accountability and the one-on-one guidance you get from a sponsor.
- SMART Recovery: If you're looking for a more science-based approach, SMART Recovery might be for you. It's a four-point program built around self-empowerment, teaching you how to build motivation, cope with urges, manage your thoughts, and find balance.
Finding the right group is a lot like finding the right pair of shoes—you might have to try on a few before one feels like a perfect fit. The goal is to land in a place where you feel safe, heard, and genuinely supported.
The Lifeline of a Sponsor or Mentor
Within many of these groups, the idea of having a sponsor or mentor is a cornerstone of the process. This is simply someone with more time and experience in recovery than you who can serve as a personal guide.
A sponsor isn't your therapist, but they can be a critical lifeline. They're the person you can text at 10 PM when a craving hits hard or call when you're wrestling with a tough emotion. They’ve already walked the path you’re on and can offer practical, real-world advice to help you get through the early days.
Mending and Managing Family Relationships
Addiction doesn't just affect you; it puts an immense strain on your relationships with the people you love. Rebuilding that trust takes time, consistency, and often, a little professional guidance. This is where family therapy can be a game-changer.
It creates a safe, mediated space for everyone to talk openly, learn about the real dynamics of addiction, and establish healthier boundaries. It helps your loved ones learn how to support you without accidentally enabling old behaviors.
The need for this kind of support system is huge. In 2021, about 22.8% of adults in the U.S. were living with a diagnosed mental illness. Yet, a staggering 47% didn't receive treatment, which underscores just how vital family understanding and access to care truly are. You can explore more of these mental health statistics on helloinnerwell.com.
How to Talk to Your Loved Ones
Bringing up your recovery with friends and family can feel incredibly awkward. You don't need a big speech; a simple, direct approach usually works best.
You could try saying something like:
- "I'm making some big changes for my health, and I've decided to stop drinking. Your support would really mean a lot to me right now."
- "I'm in recovery, and for a while, that means I need to avoid certain situations. I hope you can understand and support me in this."
These conversations open the door to setting clear boundaries, like asking friends not to drink around you or suggesting sober activities you can do together. Building this community isn't a passive activity—it's an active, ongoing process of designing a life that will protect your long-term well-being.
Creating a Relapse Prevention Plan That Actually Works
Staying sober for the long haul isn't just about white-knuckling it through cravings. It’s about consciously and deliberately building a life that feels good to live, a life you don't feel the need to escape from. One of the most critical things you can do after treatment is to create a solid relapse prevention plan.
Think of it less like a rigid set of rules and more like a personal roadmap for navigating the real world. It’s your guide for what to do when you hit those inevitable rough patches or unexpected detours. This isn't a generic template you download; it’s a plan built from an honest look at your own life and your own unique triggers.
Figure Out Your Triggers
First things first, you have to know what you’re up against. Your triggers are those specific signals—people, places, feelings, even times of day—that your brain has come to connect with using. Getting them out of your head and onto paper is the first step toward taking their power away.
- People: Is there that one friend, or a whole group, that you always used with?
- Places: Do you get a knot in your stomach driving past that one bar or a specific neighborhood?
- Feelings: Is it stress from work? Boredom on a Saturday afternoon? Or that deep ache of loneliness?
Once you’ve identified your triggers, you can start building specific, practical strategies to deal with them. For example, if that old group of friends is a trigger, your plan might be to suggest meeting for coffee instead of going out at night, or maybe you need to take a break from them for a while. If work stress is your weak spot, the plan could involve scheduling a 15-minute walk every afternoon or practicing a 5-minute breathing exercise before heading home.
A relapse prevention plan is a living document. It's not about being perfect; it's about being prepared. You're essentially giving your future self a playbook for handling tough moments with a clear head.
Your Daily Check-In: H.A.L.T.
One of the simplest yet most effective tools I’ve seen people use is the H.A.L.T. acronym. It’s a quick mental checklist to run through when you’re feeling off, agitated, or on edge. It reminds you to pause and ask yourself if you are:
- Hungry
- Angry
- Lonely
- Tired
It sounds almost too simple, but these four basic states can absolutely tank your defenses and leave you wide open to cravings. By just stopping to ask, "Am I hungry? Am I angry?" you can often pinpoint the real problem and solve it before it snowballs into an overwhelming urge to use. It's a small, practical act of self-care that can make a huge difference.
How to Think About a Relapse
This part is crucial. We need to be clear on what a relapse is—and what it isn't. A relapse is not a sign that you’re a failure or that all your hard work has been erased. It’s not a moral issue.
Think of it as a data point. A relapse is a red flag showing you that there's a weak spot in your current plan that needs to be fixed.
The single most important thing to do if you relapse is to reach out for help immediately. Don't wait. Call your sponsor, your therapist, or someone you trust in your support system. The goal is to interrupt the cycle of shame and guilt, learn from what happened, adjust your plan, and get right back on the path to recovery.
Common Questions About Starting Recovery
Taking that first step into recovery can feel like stepping into a whole new world, and it's totally normal to have a million questions. Honestly, facing these concerns head-on is one of the best ways to build the confidence you need to actually move forward.
From very real worries about how you'll pay for it to deeply personal fears about privacy and what people will think, getting straight answers is what makes this whole process feel less intimidating.
Let's walk through some of the most common questions people ask when they're thinking about the first steps to recovery. The goal here is to replace that feeling of uncertainty with real, practical clarity.
How Do I Know if My Problem Is Serious Enough for Help?
This is a big one. The simple answer is this: if substance use is negatively impacting any part of your life—your health, your job, your relationships—it's serious enough. You don't have to wait for some dramatic, life-shattering event to justify getting help.
Ask yourself a couple of honest questions. Have you tried to cut back on your own and found you couldn't? Do you ever hide how much you're using from people you care about? If you answered 'yes' to either, that’s a clear signal that professional guidance could make a huge difference. Trust your gut. If a part of you thinks it’s a problem, that’s all the reason you need.
Key Takeaway: The severity of your problem isn't measured by a "rock bottom" moment. It's measured by its impact on your quality of life. Any negative impact is a valid reason to seek help.
What Is the Difference Between Detox and Rehab?
It helps to think of your journey in two distinct phases.
Detox is the very first, short-term step. Its entire purpose is to help you safely manage the physical symptoms of withdrawal while under medical supervision. The primary job of detox is simply to get the substance out of your system without putting your health at risk.
Rehab is the next, much longer-term phase. This is where the real work begins. In rehab, you start digging into the psychological reasons behind the addiction, learn brand-new ways to cope with stress and triggers, and build a solid foundation for a life in recovery.
Put simply: detox takes care of the body, while rehab helps heal the mind.
How Can I Possibly Afford Addiction Treatment?
The cost is a massive barrier for so many people, but you almost always have more options than you think. First, most health insurance plans are required by law to cover substance abuse treatment. The best thing you can do is call the number on the back of your insurance card and ask them for a clear breakdown of your benefits.
What if you're uninsured? Don't stop there. Look into state-funded programs or non-profit centers in your area. Many of these facilities offer services on a sliding scale, meaning what you pay is based on your income. Admissions teams at treatment centers are pros at navigating these financial questions and are there to help you find a solution.
Do I Have to Tell My Boss I Am Going to Rehab?
Your privacy is protected by federal law. Thanks to regulations like the Family and Medical Leave Act (FMLA) and the Americans with Disabilities Act (ADA), you can often take a protected medical leave without having to disclose the specific reason to your boss or coworkers.
You are getting treatment for a recognized medical condition, just like any other. Your company's HR department is the place to go; they can help you arrange the leave discreetly and professionally. Your job right now is to focus on your health, and the law is there to help protect your employment while you do it.
Frequently Asked Questions (FAQ)
What is the very first step to recovery?
The very first step is acknowledging to yourself that there is a problem and that you need help. This internal admission is the most crucial part of the process because it opens the door to seeking external support and starting the journey.
How long does recovery take?
Recovery is a lifelong process, not a destination with a fixed timeline. The initial, more intensive phases like detox and inpatient rehab might last from a few days to several months, but maintaining sobriety involves ongoing commitment, self-awareness, and the use of support systems for years to come.
Can I be forced into rehab?
In some specific legal situations, such as a court order or an involuntary commitment process (which varies by state), a person can be legally mandated to attend rehab. However, for treatment to be truly effective in the long run, the individual's own motivation and willingness to change are key factors.
What happens after I finish a treatment program?
After completing a formal treatment program, the focus shifts to aftercare and relapse prevention. This typically involves continuing with therapy, participating in support groups like AA or SMART Recovery, living in a sober living environment if needed, and actively using the coping skills you learned to navigate daily life.
At StartDrugRehab.com, we are dedicated to providing the resources and support you need to confidently take the first steps toward a new life. Explore our guides and find the right path for you at https://startdrugrehab.com.

